 Those ADs that list sleep disturbance as a possible symptom include Generalized Anxiety Disorder (GAD) and Post-Traumatic Stress Disorder (PTSD) ( Belanger et al 2004). This assumption is reinforced by the fact that sleep disturbance is currently listed as a symptom of specific ADs in the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR) ( American Psychiatric Association 2000). Insomnia has traditionally been viewed as a symptom of psychiatric disorders, including ADs, rather than a stand-alone diagnosis. Further, relaxation therapy, which works to reduce anxiety and tension, is a modestly effective treatment for insomnia ( Steinmark & Borkovec 1974). Indeed, anxiety is one of the most commonly co-occurring disorders in patients complaining of insomnia ( Ford & Kamerow 1989). ADs can occur before the onset of insomnia ( Johnson et al 2006), or in other cases, the presence of a clinically significant insomnia can act as a risk factor for the future development of AD ( Ford & Kamerow 1989). In addition to subclinical levels of insomnia and/or anxiety, there is large overlap in symptoms and occurrence between those with an insomnia diagnosis and those with an anxiety disorder (AD) diagnosis. These findings suggest that experimentally inducing anxiety or poor sleep in otherwise non-anxious good sleepers can produce increases in insomnia and anxiety respectively. Likewise, artificially inducing poor sleep increases anxiety (Bonnet & Arand 1992 Talbot et al 2010). For example, artificially increasing anxiety (e.g., by telling a research participant that they will have to give a speech the following morning) results in increased sleep onset latencies, as participants experience an intrusion of unwanted and worrisome thoughts (Gross & Borkovec 1982 Hall et al 1996). This relationship is complex and reciprocal, as insomnia can precipitate anxiety and experiencing anxiety can worsen sleep. 
There are long established links between insomnia and anxiety ( Buysse et al 2006 Uhde et al 2009). In addition, the poor specificity and high number of overlapping symptoms between insomnia and anxiety highlight the diagnostic challenges facing clinicians. 
Such limitations must be considered before using this measure in insomnia patient groups. Additionally, published cutoffs for the BAI were not optimal for identifying anxiety disorders in those with insomnia. Nine items did not distinguish between those insomnia sufferers with and without an anxiety disorder. Although anxiety scores were highest in those with insomnia and an anxiety disorder, those with insomnia only had scores in the mild range for anxiety. The ROC curve analysis revealed the suggested BAI cutoff (≥16) had 55% sensitivity and 78% specificity. There were significant group differences on 12 BAI items. 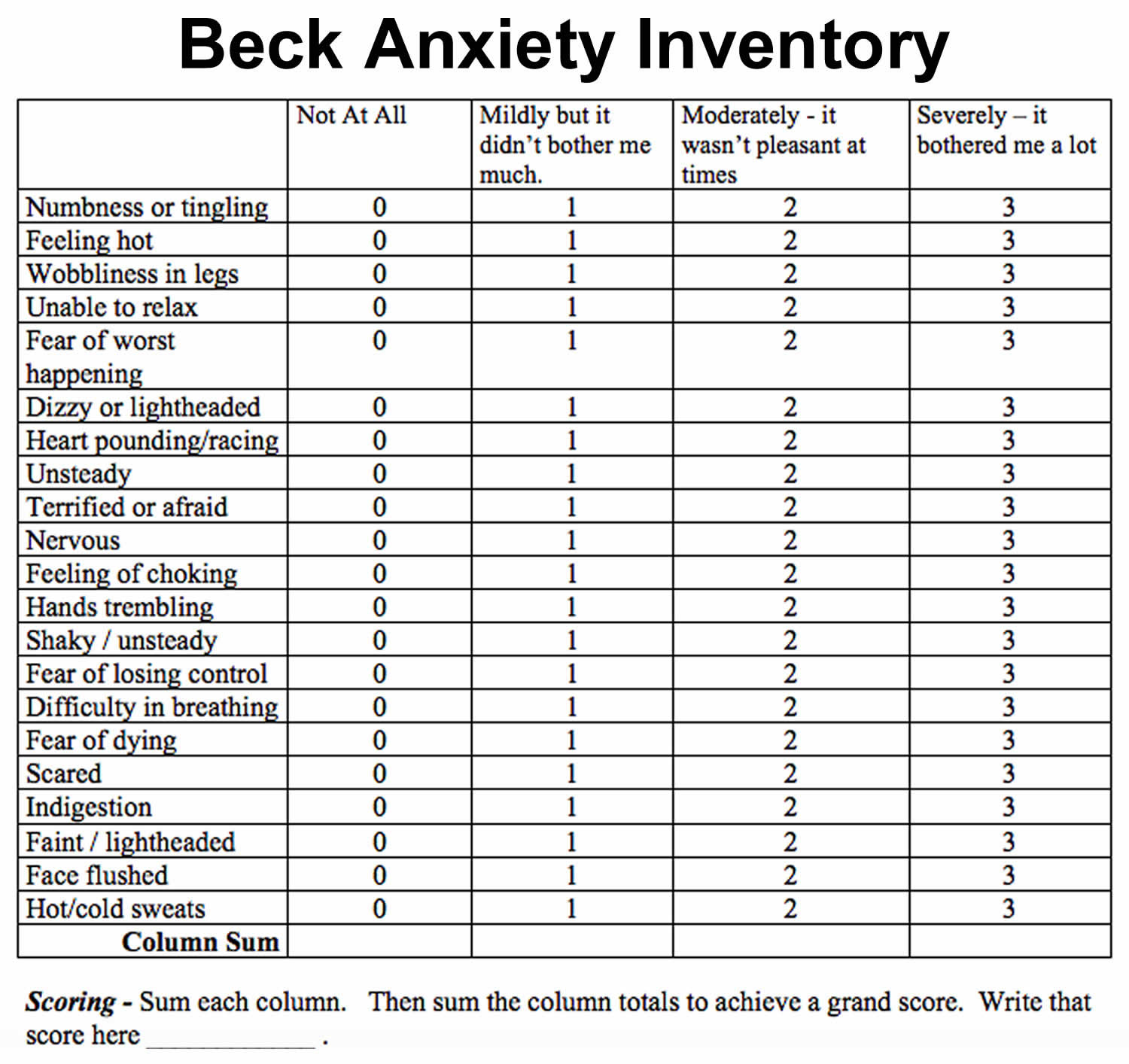
The I-ND had lower mean BAI scores than I-AD. As a validity check, a receiver operating characteristic (ROC) curve analysis was conducted to determine if the BAI suggested clinical cutoff was valid for identifying clinical levels of anxiety in this comorbid patient group. Mean Beck Anxiety Inventory (BAI) item responses were compared using multivariate analysis of variance (MANOVA) and follow-up ANOVAs. Participants ( N = 207) were classified as having insomnia: 1) without an anxiety disorder (I-ND), or 2) with an anxiety disorder (I-AD). Because of this overlap, we need studies that examine the assessment of anxiety in clinical insomnia groups. Such assessment is complex since those with Anxiety Disorders (AD) and those with PI have overlapping symptoms. Assessing for clinical levels of anxiety is crucial, as comorbid insomnias far outnumber primary insomnias (PI). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
